Are you confident that your body is getting enough oxygen and that your lungs are working properly? Knowing how to assess effective oxygenation and ventilation is crucial for your health and well-being.
When these vital processes don’t work as they should, it can lead to serious problems—sometimes without obvious signs. You’ll discover simple yet powerful ways to check if your oxygen levels and breathing are on track. By understanding these key assessments, you can take control of your respiratory health and act quickly if something feels off.
Keep reading, because your breath is more important than you might think.

Credit: www.jacc.org
Signs Of Effective Oxygenation
Signs of effective oxygenation reveal how well oxygen reaches body tissues. Checking these signs helps identify breathing or circulation problems early. Clear, quick observations guide timely care and improve outcomes.
Skin Color And Temperature
Normal skin color shows good oxygen delivery. Look for pink or light tones, not blue or pale shades. Warm skin suggests proper blood flow and oxygenation. Cold, clammy skin may signal poor oxygen supply or shock.
Pulse Oximetry Readings
Pulse oximeters measure oxygen saturation in blood. Healthy readings usually range from 95% to 100%. Levels below 90% indicate low oxygen and need for action. This tool provides fast, reliable data on oxygen levels.
Mental Status Changes
Brain function depends on oxygen. Watch for confusion, drowsiness, or restlessness. Sudden changes in alertness can mean oxygen is low. Early detection of mental changes helps prevent serious complications.
Methods To Evaluate Ventilation
Evaluating ventilation is key to understanding how well air moves in and out of the lungs. It helps to check if the body is getting enough oxygen and removing carbon dioxide properly. Several tools and observations are used to assess ventilation effectively.
Respiratory Rate And Pattern
Counting breaths per minute reveals the respiratory rate. Normal rates vary by age but usually range from 12 to 20 breaths per minute in adults. Changes in breathing rhythm or depth can signal ventilation problems. Fast, shallow breaths may indicate distress. Slow, irregular breathing might suggest lung or brain issues. Observing chest movement also helps detect abnormalities in breathing patterns.
Capnography Use
Capnography measures carbon dioxide levels in exhaled air. It provides real-time feedback on ventilation efficiency. The capnograph waveform shows how well carbon dioxide is expelled from the lungs. Normal end-tidal CO2 values range between 35-45 mmHg. Low values can mean poor lung ventilation or airway obstruction. High values may indicate hypoventilation or reduced gas exchange.
Arterial Blood Gas Analysis
Arterial blood gas (ABG) testing measures oxygen, carbon dioxide, and blood acidity. It offers detailed information about lung function. ABG shows how well oxygen enters the blood and how effectively carbon dioxide is removed. Values like PaO2, PaCO2, and pH help assess ventilation status. This test is crucial in critical care settings to guide treatment decisions.
Tools For Monitoring Oxygen Levels
Monitoring oxygen levels is vital to ensure effective oxygenation and ventilation. Various tools help track how well oxygen moves through the blood. These tools guide healthcare providers in adjusting treatments and therapies. Understanding these devices aids in better care and quick responses.
Pulse Oximeters
Pulse oximeters are common, non-invasive devices used to check oxygen levels. They clip onto a finger, toe, or earlobe and use light to measure oxygen saturation. The device displays a percentage showing how much oxygen the blood carries.
These devices provide quick results and continuous monitoring. They are easy to use and widely available in hospitals and homes. Pulse oximeters help detect low oxygen levels early, allowing timely intervention.
Oxygen Saturation Targets
Oxygen saturation targets guide treatment decisions. Normal levels typically range from 95% to 100%. Targets may vary depending on the patient’s condition and age.
For example, patients with chronic lung diseases might have lower target levels, around 88% to 92%. Maintaining proper targets avoids complications from too little or too much oxygen. Careful monitoring ensures oxygen stays within these safe limits.
Limitations Of Non-invasive Devices
Non-invasive devices like pulse oximeters have limits. They can give inaccurate readings due to poor circulation or movement. Dark skin tones, nail polish, and bright lights can also affect results.
These devices do not measure carbon dioxide levels or oxygen delivery directly. In some cases, blood gas tests are needed for a full picture. Understanding these limitations helps prevent misinterpretation of oxygen status.
Assessing Carbon Dioxide Elimination
Assessing carbon dioxide elimination is vital to ensure effective breathing and lung function. Carbon dioxide (CO2) is a waste gas produced by the body. Its removal depends on proper ventilation. Monitoring how well CO2 is expelled helps detect breathing problems early.
Both non-invasive and invasive techniques measure CO2 levels. These methods guide treatment and improve patient outcomes. Understanding signs of poor ventilation also aids in quick response.
End-tidal Co2 Monitoring
End-tidal CO2 (EtCO2) monitoring measures CO2 at the breath’s end. It reflects how well CO2 is removed from the lungs. This method uses a small sensor placed near the airway.
EtCO2 values show real-time ventilation status. Normal levels range from 35 to 45 mmHg. Low EtCO2 suggests hyperventilation or poor blood flow. High EtCO2 indicates hypoventilation or airway blockage.
This tool is common in surgery and emergency care. It is quick, painless, and continuous. It helps detect changes before symptoms appear.
Blood Gas Measurements
Blood gas tests measure CO2 and oxygen in the blood. A small blood sample is taken, usually from an artery. This test gives precise information on lung function.
Partial pressure of carbon dioxide (PaCO2) is the key value. Normal PaCO2 ranges from 35 to 45 mmHg. Elevated PaCO2 signals poor ventilation or lung disease. Low PaCO2 may show excessive breathing or anxiety.
Blood gas analysis also reveals blood pH and oxygen levels. This comprehensive data helps guide treatment decisions.
Signs Of Hypoventilation And Hyperventilation
Recognizing signs of poor ventilation is crucial for quick action. Hypoventilation means breathing too slowly or shallowly. It causes CO2 buildup in the body. Symptoms include:
- Confusion or drowsiness
- Headache
- Slow, shallow breaths
- Increased heart rate
Hyperventilation means breathing too fast or deeply. It lowers CO2 levels too much. Symptoms include:
- Dizziness or lightheadedness
- Numbness or tingling in fingers
- Rapid breathing
- Chest tightness
Early recognition allows for timely interventions. Monitoring and clinical signs together ensure effective patient care.
Clinical Techniques For Ventilation Assessment
Effective oxygenation and ventilation are assessed by checking breathing rate, chest movement, and oxygen levels in the blood. Listening to lung sounds and observing skin color also help evaluate respiratory function. These steps ensure the body gets enough oxygen and removes carbon dioxide properly.
Assessing ventilation in clinical settings is crucial for ensuring patients receive adequate oxygen and maintain healthy respiratory function. Various techniques help healthcare professionals evaluate how effectively a patient’s lungs are working. Understanding these methods can empower you to recognize potential issues early and seek appropriate medical advice.Auscultation Of Breath Sounds
Listening to breath sounds is a fundamental skill for assessing ventilation. By using a stethoscope, healthcare providers can detect abnormal sounds like wheezing, crackles, or diminished breath sounds. Each of these can indicate different underlying issues, such as airway obstruction or fluid in the lungs. Have you ever noticed how a mechanic can tell what’s wrong with a car just by listening to the engine? Similarly, trained ears can pick up subtle differences in breath sounds, pointing to specific respiratory conditions.Observation Of Chest Movement
Visual observation is another key method. Watching the rise and fall of a patient’s chest provides insights into their breathing pattern and effort. Irregular or asymmetrical chest movements might suggest problems like pneumothorax or diaphragmatic dysfunction. This technique is non-invasive and can be performed quickly, making it an essential tool in emergency situations. Imagine standing by a calm lake. The gentle, rhythmic waves reflect the breath of the wind—just as your chest movements mirror your breathing patterns. Any disturbance can signal a change that needs attention.Use Of Ventilator Waveforms
In settings where patients are on mechanical ventilation, ventilator waveforms become indispensable. These graphical representations show real-time data on various parameters like pressure, volume, and flow. By analyzing these waveforms, clinicians can make necessary adjustments to the ventilator settings, ensuring optimal support for the patient. It’s like having a dashboard full of gauges in a car. Each waveform provides crucial information about the patient’s respiratory status, allowing for precise tuning of the ventilator settings. These techniques, when used together, form a comprehensive approach to ventilation assessment. By understanding and applying them, you can ensure the best possible care for patients in need.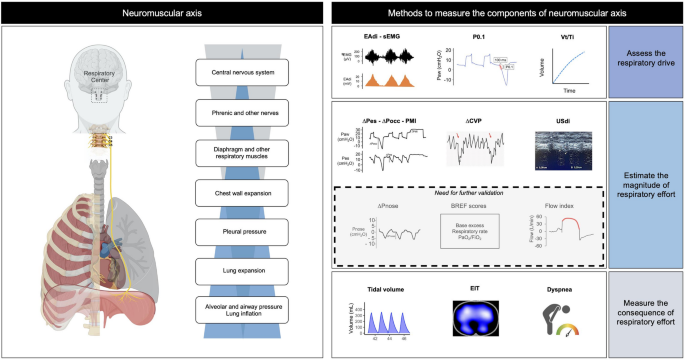
Credit: ccforum.biomedcentral.com
Integrating Assessment Data
Integrating assessment data is key to understanding how well oxygenation and ventilation are working in a patient. It means looking beyond isolated numbers and clinical signs and seeing the whole picture. This approach helps you make smarter decisions about care and quickly spot when something is off.
Combining Clinical Signs With Monitoring Results
Clinical signs like skin color, breathing effort, and mental alertness tell you a lot about a patient’s oxygen and ventilation status. But these signs alone can be misleading or subtle. That’s why you should always compare them with monitoring tools such as pulse oximetry, capnography, and arterial blood gases.
For example, a patient might look comfortable but have a low oxygen saturation reading on the monitor. Or you might see fast breathing but normal carbon dioxide levels. Checking both clinical signs and monitor data together gives you a clearer, more reliable assessment.
Adjusting Interventions Based On Findings
Once you combine all the data, you can tailor your interventions effectively. If oxygen levels are low but breathing effort is strong, increasing oxygen flow might be enough. But if ventilation is inadequate, you may need to consider assisted breathing or other support.
Always ask yourself: What does the combined data tell me about the patient’s current state? How urgent is the intervention? This mindset helps avoid unnecessary treatments or delays in care.
Remember, continuous reassessment is crucial. Patient conditions can change quickly, so keep checking both signs and monitor readings to adjust your approach in real time.

Credit: www.jacc.org
Frequently Asked Questions
What Are The Key Signs Of Effective Oxygenation?
Effective oxygenation is indicated by normal oxygen saturation (SpO2) levels above 95%. Pink skin color and normal respiratory rate also signal good oxygenation. Pulse oximetry is commonly used to monitor oxygen levels continuously and non-invasively.
How Is Ventilation Effectiveness Measured Clinically?
Ventilation effectiveness is assessed by measuring carbon dioxide levels in the blood (PaCO2). Normal PaCO2 ranges from 35 to 45 mmHg. Capnography is a non-invasive tool that tracks end-tidal CO2, reflecting ventilation status in real-time.
Why Monitor Both Oxygenation And Ventilation Together?
Monitoring both ensures adequate gas exchange and respiratory function. Oxygenation shows how well oxygen reaches tissues, while ventilation removes carbon dioxide. Assessing both helps detect respiratory issues early and guides appropriate treatment.
What Tools Assess Oxygenation In Patients?
Pulse oximeters and arterial blood gas (ABG) tests are primary tools. Pulse oximetry measures peripheral oxygen saturation non-invasively. ABG provides detailed oxygen, carbon dioxide, and blood pH levels for comprehensive assessment.
Conclusion
Effective oxygenation and ventilation keep the body healthy. Checking breathing rate and oxygen levels helps assess them. Doctors use tools like pulse oximeters and blood gas tests. Watching chest movements and listening to breath sounds give clues too. Quick action improves patient care and prevents problems.
Understanding these signs helps you stay safe and informed. Keep learning about your body’s needs. Good oxygen and ventilation mean better health every day. Simple steps make a big difference. Stay aware and take care.