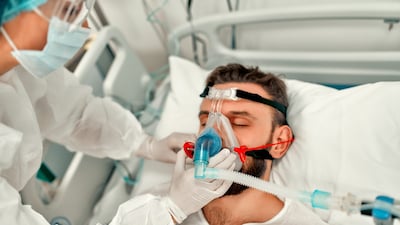
Have you ever wondered how long someone can stay on a ventilator? If you or a loved one is facing this situation, it’s natural to feel anxious and full of questions.
Understanding the facts can help ease your mind and prepare you for what lies ahead. You’ll discover what determines the length of time on a ventilator and what it means for recovery. Keep reading to get clear answers that matter to you.
Ventilator Basics
Understanding the basics of ventilators is essential if you or a loved one faces a situation requiring mechanical breathing support. Ventilators play a crucial role in helping people breathe when their lungs can’t do the job alone. Knowing how these machines work can ease your concerns and help you engage more confidently with healthcare providers.
What A Ventilator Does
A ventilator is a machine designed to assist or replace spontaneous breathing. It pushes air into your lungs through a tube placed in your airway, ensuring your body gets enough oxygen and removes carbon dioxide.
Sometimes, your lungs may be too weak or damaged to function properly. The ventilator takes over the work of breathing, giving your lungs a chance to heal. Have you ever wondered how this invisible lifeline can keep someone alive when they can’t breathe on their own?
Types Of Ventilators
Not all ventilators are the same. Different types are used depending on your specific medical needs and the severity of your condition.
- Invasive Ventilators:These use a tube inserted into your windpipe. They provide full breathing support and are common in intensive care units.
- Non-invasive Ventilators:These use masks that fit over your nose or mouth. They are often used for less severe breathing problems.
- Portable Ventilators:Small and lightweight, these allow mobility for patients who still need breathing assistance but want some freedom.
Choosing the right ventilator depends on many factors, including your lung function, comfort, and how long you might need support. Have you ever thought about how technology adapts to meet such critical needs in healthcare?

Credit: medium.com
Factors Affecting Duration
Several factors influence how long a person stays on a ventilator. These factors impact the body’s ability to breathe independently. Understanding them helps in predicting the duration of ventilation support.
Underlying Health Conditions
Chronic diseases like lung or heart problems can extend ventilator use. Damaged lungs need more time to heal and recover. Patients with weak immune systems face higher risks of complications. This often leads to longer ventilation periods. Health conditions such as diabetes or kidney failure also slow recovery.
Severity Of Illness
Severe illnesses require longer breathing support. Conditions like pneumonia or severe COVID-19 cause serious lung damage. The body struggles to get enough oxygen on its own. Critical cases may need ventilation for weeks or even months. Mild cases often allow quicker weaning from the ventilator.
Patient Age And Strength
Older patients generally need more time on a ventilator. Aging reduces lung function and muscle strength. Younger people tend to recover faster and breathe independently sooner. Muscle weakness from long hospital stays can delay breathing recovery. Stronger patients have a better chance of early ventilator removal.
Typical Ventilation Periods
Understanding how long a person can be on a ventilator is crucial, especially if you or a loved one faces serious health challenges. The length of ventilation varies widely depending on the individual’s condition and recovery process. Here’s a clear look at typical ventilation periods to help you grasp what to expect.
Short-term Use
Short-term ventilation usually lasts from a few hours to several days. It often happens after surgery or during a sudden illness where breathing support is needed temporarily.
Patients who undergo routine surgeries may wake up with a ventilator but are typically weaned off quickly. This brief use helps ensure their lungs work properly as anesthesia wears off.
Have you ever wondered why some people recover so fast while others stay on a ventilator longer? The key is how quickly their lungs regain strength and the absence of complications like infections.
Long-term Use Scenarios
Long-term ventilation can last weeks, months, or even years. This occurs when a patient’s lungs or respiratory muscles are severely damaged or weakened.
People with chronic illnesses like COPD, spinal cord injuries, or certain neuromuscular diseases often require prolonged ventilator support. At times, a tracheostomy is performed to make long-term ventilation more comfortable and safer.
Living on a ventilator for a long time raises questions about quality of life and ongoing care. How do medical teams balance life support with patient comfort and independence? Understanding these scenarios can prepare you for the challenges ahead.

Credit: goodmenproject.com
Risks Of Prolonged Ventilation
Spending an extended time on a ventilator can save lives, but it also brings serious risks. Understanding these risks helps you prepare and ask the right questions about care options. The longer ventilation lasts, the more your body faces challenges beyond the initial illness.
Infections And Complications
One of the biggest dangers of prolonged ventilation is infection. Breathing tubes can introduce bacteria into your lungs, increasing the risk of pneumonia. This isn’t just a minor issue; ventilator-associated pneumonia can significantly delay recovery and even be life-threatening.
Beyond pneumonia, other complications include blood clots, pressure sores, and damage to the airway from the tube itself. You might wonder how hospitals prevent these risks. They use strict hygiene protocols and regularly assess the need to keep the ventilator on, but infections can still happen.
Muscle Weakness And Lung Damage
Your muscles, including those that help you breathe, can weaken when a ventilator does the work for too long. This makes it harder to wean off the machine because your body needs to rebuild strength. Some patients describe feeling like their body has forgotten how to breathe on its own.
Additionally, the lungs can suffer damage from the pressure and oxygen levels used during ventilation. This damage might lead to scarring or reduced lung function over time. Have you thought about how this might affect your quality of life after leaving the hospital?
Weaning Off The Ventilator
Determining how long a person can stay on a ventilator depends on their condition and recovery rate. Some individuals require weeks or even months, while others may need just a few days. Medical teams continuously assess each patient to decide the best time for weaning off.
Weaning off the ventilator is a crucial step in a patient’s journey toward recovery. It involves gradually reducing the ventilator support as the patient regains the ability to breathe independently. This process can be complex and requires careful monitoring and assessment by healthcare professionals.Signs For Weaning
Knowing when to start weaning is essential. Healthcare providers look for certain signs indicating a patient is ready. These include improved respiratory strength and the ability to follow simple commands. Your loved one might also show increased alertness and a strong cough, which are positive indicators. It’s important to remember that each patient’s journey is unique, and progress can vary.Weaning Methods And Challenges
Various methods can be employed for weaning. The most common is the gradual reduction of ventilator support, allowing the patient to breathe more on their own. Some patients might benefit from a “spontaneous breathing trial,” where they breathe without assistance for short periods. Challenges can arise during weaning, such as patient anxiety or fluctuations in vital signs. Have you ever wondered how you can support someone facing these challenges? Encouragement and patience can make a significant difference. Your support can help them stay motivated and reduce anxiety during this critical phase.Recovery After Ventilation
Recovery after being on a ventilator is a complex journey that goes beyond just breathing on your own again. Your body and mind need time and care to regain strength and balance. Understanding what lies ahead can help you prepare and actively participate in your healing process.
Physical Rehabilitation
After ventilation, your muscles, especially those involved in breathing, may feel weak. Starting physical rehabilitation early can make a big difference in how quickly you regain your strength.
Rehabilitation often includes:
- Breathing exercises to improve lung function
- Gentle stretching and movement to rebuild muscle strength
- Gradual increase in activity levels to avoid overwhelming your body
Think about how small daily steps, like sitting up or walking a few steps, can build your endurance. Have you considered how your body responds to these activities and what progress you can celebrate every day?
Emotional And Psychological Support
Being on a ventilator can be frightening and isolating, leaving emotional scars that need attention. It’s normal to feel anxious, confused, or even depressed after such an experience.
Support can come from:
- Counseling or therapy to process your feelings
- Support groups where you connect with others who have been through similar experiences
- Family and friends offering encouragement and understanding
Addressing your mental health is just as important as physical recovery. Are you open to sharing your feelings with someone who can help you navigate this challenging time?
Advances In Ventilator Care
Ventilator care has seen major improvements in recent years. These advances help patients breathe better and recover faster. Medical teams now have more tools and knowledge to support patients on ventilators safely. Technology and care methods continue to evolve, making long-term ventilation more manageable.
Innovative Technologies
New ventilators use smart sensors to adjust airflow automatically. They respond to the patient’s breathing patterns in real time. Portable ventilators allow more flexibility outside hospitals. Advanced filters reduce infection risks. Software updates improve machine accuracy and safety. These innovations help tailor breathing support for each patient’s needs.
Improved Patient Outcomes
Better ventilator care reduces lung injuries and complications. Early detection systems alert doctors to breathing problems quickly. Physical therapy combined with ventilation supports muscle strength. Care teams focus on minimizing sedation to keep patients alert. These practices lead to shorter ventilation times and faster recovery. Patients experience fewer side effects and better overall health.
Credit: www.agapehospicepc.org
Frequently Asked Questions
How Long Can A Person Stay On A Ventilator?
A person can stay on a ventilator from a few days to several weeks. Duration depends on illness severity and recovery speed. Doctors regularly assess to minimize risks and decide when to wean off the ventilator safely.
What Factors Affect Ventilator Duration?
Factors include the underlying illness, lung function, overall health, and response to treatment. Complications like infections can prolong ventilator use. Each patient’s condition is unique, influencing how long mechanical ventilation is necessary.
Can Long-term Ventilator Use Cause Complications?
Yes, long-term use can cause lung damage, infections, and muscle weakness. Prolonged ventilation increases risks, so medical teams monitor patients closely to manage and reduce potential complications.
How Do Doctors Decide To Remove A Ventilator?
Doctors assess breathing ability, oxygen levels, and overall health. They conduct spontaneous breathing tests and monitor for stability. Removal happens when patients can breathe independently and safely without mechanical support.
Conclusion
Time on a ventilator varies for each person. Doctors decide based on health and recovery. Some need a few days, others weeks or months. Staying on a ventilator can have risks. But it also helps many breathe when they cannot.
Families should stay informed and ask questions. Medical teams work hard to help patients heal. Patience and care are very important during this time. Understanding the process can ease worries and fears. Every case is unique, and hope remains strong.