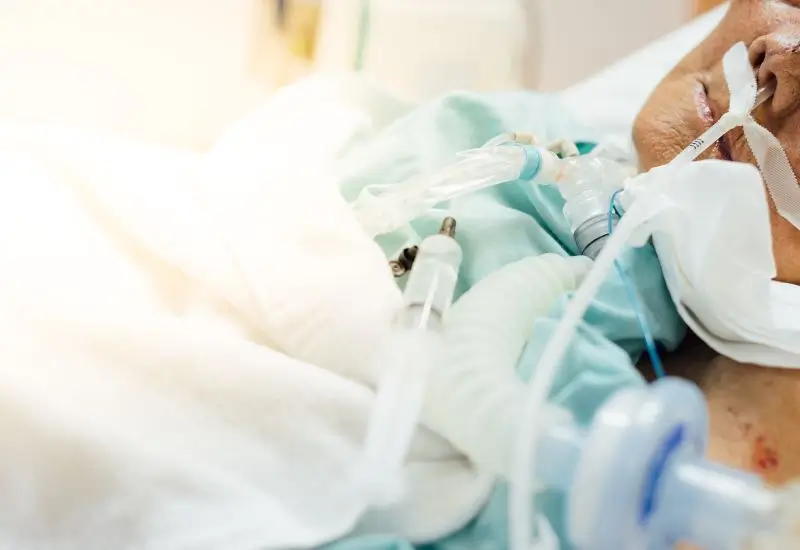
Have you ever wondered how long someone can live on a ventilator? If you or a loved one is facing this situation, the uncertainty can be overwhelming.
Understanding what a ventilator does and how it affects life expectancy can help you feel more in control. You’ll discover clear answers and important facts that can ease your worries and prepare you for what’s ahead. Keep reading to learn what you need to know about living on a ventilator.

Credit: www.theguardian.com
Ventilator Basics
Understanding the basics of ventilators is key if you or a loved one ever face respiratory challenges. Ventilators are medical devices that support or replace breathing when the lungs can’t do the job alone. Knowing how they work and why they’re used can help you feel more informed and prepared during a difficult time.
What Is A Ventilator?
A ventilator is a machine that helps move air in and out of your lungs. It delivers oxygen and removes carbon dioxide when your breathing is too weak or irregular.
Think of it as a mechanical assistant for your lungs, taking over the work of breathing when your body can’t keep up.
Types Of Ventilators
There are several types of ventilators, each designed for different needs:
- Invasive Ventilators:These require a tube inserted into the windpipe. They are used in critical cases where complete breathing support is necessary.
- Non-invasive Ventilators:These use masks or nasal prongs to help with breathing. They’re often used for less severe respiratory issues or during recovery.
- Portable Ventilators:Small and lightweight, these allow patients to move around outside the hospital.
Choosing the right type depends on your condition and how much breathing support you need.
When Is Ventilator Support Needed?
Ventilator support becomes necessary when your lungs cannot provide enough oxygen or remove carbon dioxide effectively. This can happen due to:
- Severe lung infections like pneumonia
- Chronic respiratory diseases such as COPD
- Trauma or surgery affecting breathing muscles
- Neurological conditions impairing respiratory control
Have you ever wondered what it feels like to rely on a machine to breathe? It’s a powerful reminder of how vital your lungs are, and how medical technology can save lives when they struggle.
Duration On A Ventilator
Understanding the duration someone can live on a ventilator is vital for patients and their families. The length of time varies widely based on the purpose of ventilation and the patient’s overall health. Let’s break down what short-term and long-term ventilator use looks like, along with key factors influencing how long it may last.
Short-term Use
Short-term ventilation usually lasts from a few hours to several days. It often supports patients recovering from surgeries, severe infections, or acute respiratory issues. Many people come off the ventilator quickly once their lungs regain strength.
Think about a friend who underwent surgery and spent a night on a ventilator. They woke up breathing on their own the next day. This shows how ventilators provide temporary support during critical moments.
Long-term Use
Long-term ventilation extends beyond weeks or months and may continue for years in some cases. It’s common for people with chronic lung diseases, spinal cord injuries, or neuromuscular conditions. Living on a ventilator long-term requires specialized care and lifestyle adjustments.
Imagine someone managing a chronic condition, relying on a ventilator at home. Their experience highlights the importance of equipment maintenance, caregiver support, and regular medical check-ups to maintain quality of life.
Factors Affecting Duration
Several factors influence how long a person stays on a ventilator:
- Underlying illness:Some diseases heal quickly, others progress slowly or worsen.
- Age and overall health:Younger, healthier individuals may recover faster.
- Complications:Infections or lung damage can extend the need for ventilation.
- Ventilator settings and type:Different modes and machines suit different needs.
Have you considered how these factors might apply to your own health situation or that of a loved one? Being aware can prepare you for discussions with healthcare providers and help you set realistic expectations.
Health Impacts Of Ventilator Use
Using a ventilator can be a life-saving measure, but it also comes with various health impacts you should be aware of. Understanding these effects helps you prepare for what lies ahead and take an active role in care decisions. Let’s look closely at what using a ventilator means for your body and mind.
Potential Complications
Ventilators can cause issues like lung infections or damage to lung tissue from prolonged pressure. You might experience pneumonia, especially if bacteria enter through the breathing tube. Muscle weakness is common too, since your breathing muscles can get lazy when the ventilator does the work.
Another concern is airway injury, which can occur due to the tube placement. You may also face complications like blood clots or lung collapse. Knowing these risks helps you watch for warning signs and communicate effectively with your care team.
Physical And Emotional Effects
Physically, being on a ventilator can make you feel weak and tired. Your muscles, including those used for breathing, may lose strength quickly. This can make the transition off the ventilator harder than expected.
Emotionally, you might feel isolated or anxious because you can’t speak easily or move freely. Some people report feelings of confusion or fear during ventilation. It’s important to address these feelings with your healthcare providers or loved ones to find comfort and reassurance.
Preventing Ventilator-associated Issues
You can reduce risks by keeping the breathing tube clean and ensuring proper oral hygiene. Frequent repositioning helps prevent pressure sores and lung complications. Healthcare teams often use specific protocols to minimize infections and muscle loss.
Ask about early physical therapy to keep your muscles active. Simple exercises, even while on the ventilator, can speed up recovery. Staying informed and involved can make a big difference in your outcomes.
Outcomes And Survival Rates
Understanding the outcomes and survival rates of living on a ventilator can help you make informed decisions about care and expectations. Survival varies widely based on the underlying condition, age, and overall health. Let’s look closely at what the numbers say, what recovery might look like, and how life changes after ventilation.
Survival Statistics
Survival rates for patients on a ventilator depend heavily on the reason for ventilation. For acute conditions like pneumonia or surgery recovery, survival can be as high as 70-80%. Chronic illnesses or severe neurological damage tend to lower these rates significantly.
Research shows that:
- About 50% of patients ventilated for respiratory failure survive beyond 6 months.
- Long-term ventilation (beyond 21 days) survival rates drop to around 30-40%.
- Older adults and those with multiple health issues face lower survival chances.
Have you ever wondered how these numbers translate to real life? Knowing your specific situation can help clarify what to expect.
Recovery Possibilities
Recovery after ventilation varies. Some patients breathe independently within days or weeks. Others require prolonged support or transition to home ventilators.
Key factors influencing recovery include:
- The underlying illness or injury causing respiratory failure.
- The patient’s strength and immune system.
- Timely and appropriate medical care.
It’s important to ask your care team about rehabilitation options. Physical therapy and respiratory exercises can improve your chances of weaning off the ventilator sooner.
Quality Of Life After Ventilation
Living on or after ventilation often means adjustments. Some regain full independence, while others face challenges like muscle weakness or cognitive effects.
Consider these points about life post-ventilation:
- Many patients need ongoing respiratory support at home.
- Emotional and psychological support is vital to cope with changes.
- Regular follow-ups help manage complications and improve wellbeing.
How would you prepare yourself or a loved one for these changes? Planning ahead can ease the transition and improve daily life quality.
Weaning Off The Ventilator
Living on a ventilator depends on health and care quality. Some people breathe with help for weeks or months. Weaning off means slowly reducing support until breathing alone is possible.
Weaning off a ventilator is a significant step in recovery. It involves transitioning from machine-assisted breathing to natural breathing. This process requires careful planning and monitoring. For patients and families, understanding this journey is crucial.Criteria For Weaning
Not every patient is ready to leave the ventilator. Doctors consider several factors before starting the weaning process. The patient must be stable. Their underlying condition should be improving. They should show signs of adequate oxygenation and ventilation. The patient’s ability to breathe on their own is assessed. This involves checking muscle strength and mental alertness. The medical team evaluates these factors continuously.Weaning Process
The weaning process is gradual. It starts with reducing ventilator support. This allows the patient to do more of the breathing work. Doctors use tests to see how well the patient copes. One common method is the spontaneous breathing trial. During this trial, the ventilator provides minimal assistance. The patient’s breathing effort and comfort are closely monitored.Challenges During Weaning
Weaning can present several challenges. Some patients experience anxiety or fear. Breathing without assistance can be tiring. The patient might feel breathless or fatigued. Medical teams provide support to ease these feelings. They adjust the weaning process based on the patient’s response. Communication between patient, family, and healthcare providers is vital. This ensures everyone understands the goals and progress. Understanding these elements can help ease the weaning journey. It is essential for a successful return to natural breathing.
Credit: www.nejm.org
Caregiver And Family Role
Caring for a loved one on a ventilator is a demanding role. Families and caregivers provide essential help beyond medical needs. Their involvement improves the patient’s comfort and quality of life. Support from family creates a positive environment for recovery and coping.
Emotional Support
Patients on ventilators often feel scared and isolated. Caregivers offer comfort through presence and kind words. Listening patiently helps patients express fears and worries. Small gestures, like holding a hand, bring calm and reassurance. Emotional support can reduce stress and improve well-being.
Monitoring And Communication
Caregivers watch for changes in breathing and overall health. They learn to recognize signs that need medical attention. Clear communication with healthcare providers is vital. Keeping detailed notes helps track progress and concerns. Families act as advocates, ensuring the patient’s needs are met.
Planning For Long-term Care
Ventilator use can last days, months, or years. Planning for the future protects the patient’s comfort and safety. Families explore options like home care or specialized facilities. Preparing the home with proper equipment is important. Discussing legal and financial matters early eases stress later.
Credit: www.themarshallproject.org
Frequently Asked Questions
How Long Can A Person Survive On A Ventilator?
Survival on a ventilator varies widely depending on health and illness. Some live days, others months or years with care. Long-term ventilation requires monitoring to prevent complications and improve quality of life. Outcomes depend on the underlying condition and overall health.
What Factors Affect Ventilator Survival Time?
Age, underlying disease, and overall health strongly impact ventilator survival. Severity of lung injury and response to treatment also matter. Proper care and infection prevention can extend survival. Each patient’s situation is unique, influencing how long they can remain on a ventilator.
Can Someone Live Years On A Ventilator?
Yes, some patients live years on ventilators with proper medical support. Chronic respiratory failure or neuromuscular diseases often require long-term ventilation. Quality of life and complications are key concerns. Advances in care have improved long-term survival rates for ventilated patients.
What Complications Shorten Ventilator Survival?
Common complications include infections, lung damage, and muscle weakness. Ventilator-associated pneumonia is a major risk. Prolonged use can cause airway injury and respiratory muscle atrophy. Managing these risks is critical to extend survival and improve patient outcomes.
Conclusion
Living on a ventilator depends on many factors. Each person’s health and condition differ greatly. Some live for weeks, others for months or years. Medical care and support play a big role. Quality of life matters most in these cases.
Families and doctors work together every day. Understanding this helps prepare for tough decisions. Breathing machines save lives but don’t cure illness. Hope and patience remain important throughout the journey. Life on a ventilator can be complex and unique.