If you or a loved one is facing pneumonia, you might be worried about the time spent on a ventilator. You probably have many questions: How long will the breathing machine be needed?
What does this mean for recovery? Understanding what to expect can ease your fears and help you prepare. You’ll discover clear answers about ventilator use for pneumonia, why the duration varies, and what factors influence your journey back to health.
Keep reading to gain the insight and confidence you need during this challenging time.
Ventilator Use In Pneumonia
Ventilator use in pneumonia is a critical topic because it directly impacts recovery and survival rates. Pneumonia can severely impair your lungs’ ability to supply oxygen to your body, sometimes requiring mechanical help. Understanding when and how ventilators are used helps you grasp the seriousness of the condition and what to expect during treatment.
When Ventilation Becomes Necessary
You might wonder, at what point does pneumonia push someone onto a ventilator? It usually happens when your lungs can no longer provide enough oxygen or remove carbon dioxide effectively. This condition is called respiratory failure.
Doctors look for signs such as:
- Severe shortness of breath despite oxygen therapy
- Confusion or drowsiness caused by low oxygen levels
- Rapid breathing or high heart rate that doesn’t improve
Imagine your lungs as filters that fail to let enough air through. At that moment, a ventilator steps in to do the breathing for you until your lungs heal enough to work on their own.
Types Of Ventilators Used
Not all ventilators are the same. Different types serve different needs depending on how severe the pneumonia is and the patient’s condition.
| Type of Ventilator | How It Works | When It’s Used |
|---|---|---|
| Non-invasive Ventilation (NIV) | Delivers air through a mask without surgery | Mild to moderate respiratory distress |
| Invasive Mechanical Ventilation | Uses a tube inserted into the windpipe | Severe respiratory failure or unconscious patients |
Knowing these types helps you understand why a doctor might recommend a mask first but switch to a tube if things worsen. It’s about using the least invasive method that keeps you safe and comfortable.
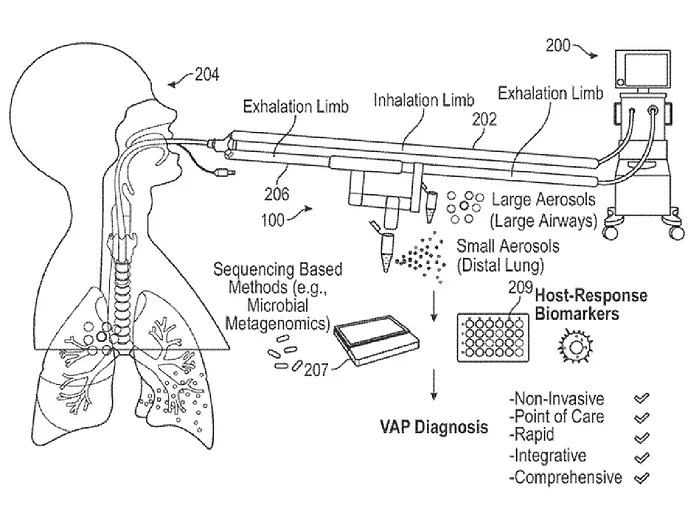
Credit: www.bioworld.com
Factors Influencing Ventilation Duration
The length of time a patient spends on a ventilator due to pneumonia varies widely. Several key factors influence this duration, shaping the recovery path and the care required. Understanding these factors can help you better prepare for what lies ahead and engage in conversations with healthcare providers.
Severity Of Pneumonia
The more severe the pneumonia, the longer you can expect the need for ventilator support. Severe cases often involve extensive lung infection and inflammation, making it harder for the lungs to function properly. If your lungs are seriously compromised, the ventilator helps keep oxygen flowing while your body fights the infection.
Think about a friend who was on a ventilator for weeks due to aggressive pneumonia. His lungs needed extra time to heal, illustrating how severity directly affects ventilation duration. Have you ever wondered why some patients bounce back quickly, while others stay on support longer? Severity is a big part of that answer.
Patient Age And Health
Your age and overall health play a huge role in how quickly you recover. Younger and healthier individuals often breathe easier once treatment begins, shortening ventilator time. In contrast, older adults or those with weakened immune systems might need more prolonged support.
Chronic illnesses like diabetes or heart disease can slow recovery. These conditions can weaken your body’s ability to fight infection and heal damaged lung tissue. If you or a loved one faces such health challenges, it’s vital to prepare mentally and practically for possibly longer ventilation.
Complications And Coexisting Conditions
Complications like lung abscesses, sepsis, or organ failure can extend ventilator use significantly. These issues add complexity to treatment and delay lung recovery. Even if pneumonia is under control, other medical problems might keep you on the ventilator longer.
Coexisting conditions like COPD or asthma also impact breathing and recovery speed. Managing these alongside pneumonia requires careful coordination and often affects ventilator duration. Have you considered how multiple health issues might change your or a loved one’s treatment timeline?
Typical Ventilation Timeframes
Typical ventilation timeframes for pneumonia vary based on illness severity and patient response. Ventilators support breathing when lungs cannot function properly. The duration on a ventilator depends on many factors including infection severity, lung damage, and overall health. Understanding typical timeframes helps patients and families prepare for the recovery process.
Average Duration For Mild Cases
Mild pneumonia cases usually require shorter ventilation times. Patients often need support for a few days up to one week. During this time, antibiotics and treatments help clear the infection. Lung function improves steadily as inflammation decreases. Doctors monitor breathing closely to remove the ventilator as soon as possible. Early removal reduces risks of complications like infections or muscle weakness.
Extended Ventilation In Severe Cases
Severe pneumonia can cause extensive lung damage. Ventilation support may last for several weeks or longer. Patients often need extra care to manage complications. Prolonged ventilation increases the risk of lung scarring and muscle loss. Recovery is slow and requires rehabilitation after ventilator removal. Doctors adjust treatment based on daily progress and lung healing.
Monitoring And Adjusting Ventilation
Monitoring and Adjusting Ventilation Ventilator support for pneumonia varies with each patient. Regular monitoring ensures effective breathing. Adjustments are made based on oxygen levels and lung improvement.
Monitoring and adjusting ventilation for pneumonia patients is crucial. It’s a delicate process. Doctors closely watch every breath. They use advanced machines to help the lungs. The goal is to ensure enough oxygen while supporting recovery. It requires constant attention.Signs Of Improvement
Doctors look for signs of improvement daily. Increased lung function is a positive sign. More stable vital signs indicate progress. Reduced need for high oxygen levels is encouraging. Patients may also show better alertness. These are all promising signs.Weaning Process From The Ventilator
Weaning starts when the patient shows improvement. Doctors gradually reduce ventilator support. They watch for any distress signs. A slow and steady process is safer. Patients may breathe on their own for short periods. This helps their lungs regain strength. The goal is to remove the ventilator fully.Recovery After Ventilation
Recovering after being on a ventilator for pneumonia can be a challenging journey. Your body needs time and support to regain strength and function. Understanding what comes next helps you prepare for the road to full recovery.
Physical Rehabilitation
After ventilation, your muscles may feel weak, especially those used for breathing and movement. Physical rehabilitation focuses on rebuilding your strength gradually.
Therapists often guide you through exercises that improve lung capacity and overall mobility. Even simple activities like sitting up or walking short distances can make a big difference.
Have you noticed how small improvements in movement can boost your confidence? Staying consistent with rehab exercises speeds up recovery and helps you regain independence faster.
Psychological Support
Being on a ventilator can be a frightening experience, and it’s common to feel anxious or depressed afterward. Psychological support is essential to address these feelings.
Talking to a counselor or joining a support group can help you process your experience. You’re not alone—many people find that sharing their story reduces stress and improves mental health.
How are you coping emotionally after your time on the ventilator? Paying attention to your mental well-being is just as important as physical healing.

Credit: goodmenproject.com
Risks And Complications Of Ventilator Use
Using a ventilator can save lives for pneumonia patients. Still, it comes with certain risks and complications. Understanding these risks helps families and patients prepare for possible challenges.
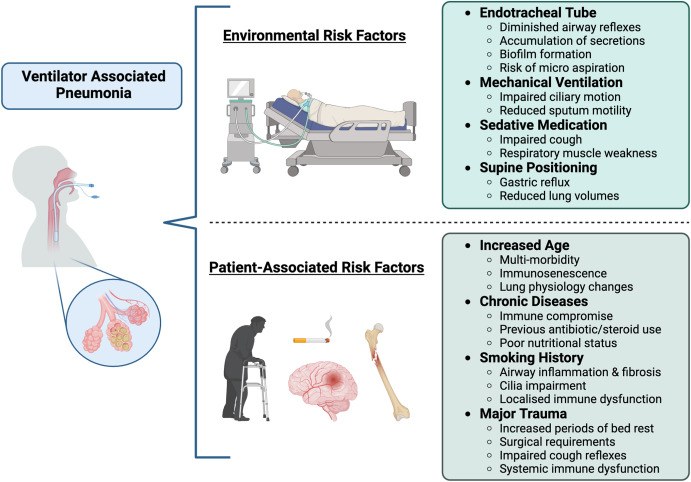
Ventilator-associated Pneumonia
Ventilator-associated pneumonia (VAP) is a common risk. It happens when bacteria enter the lungs through the breathing tube. This infection can make recovery harder and longer.
Hospitals try to prevent VAP by:
- Keeping the breathing tube clean
- Using sterile techniques
- Regularly checking lung health
Early detection and treatment are crucial to avoid serious problems from VAP.
Lung Injury And Other Risks
Ventilators can cause lung injury due to pressure or volume changes. This can lead to inflammation and scarring of lung tissue.
Other risks include:
- Damage to the vocal cords from the tube
- Muscle weakness from prolonged ventilation
- Blood clots due to immobility
- Delirium or confusion in some patients
Doctors monitor patients closely to reduce these risks during ventilation.
Tips For Families And Caregivers
When a loved one is on a ventilator due to pneumonia, the experience can be overwhelming for families and caregivers. Knowing how to support recovery and communicate effectively with healthcare providers can make a significant difference. These tips will help you stay involved and provide the best care possible during this challenging time.
Supporting Recovery
Your presence and encouragement can boost your loved one’s spirits. Simple actions like holding their hand or talking softly can help them feel less isolated. Remember, recovery isn’t just physical—it’s emotional too.
Ask the healthcare team about ways you can assist with daily care routines. This might include helping with breathing exercises or encouraging small movements when possible. These small steps can speed up healing and improve lung function.
Pay attention to signs of discomfort or confusion, and share these observations with the medical staff. Your insights can help tailor care to your loved one’s needs. Have you noticed any changes after visits or treatments?
Communicating With Healthcare Providers
Clear communication with doctors and nurses is essential. Prepare questions ahead of time to make the most of your conversations. Write down updates, medication changes, and care instructions to avoid confusion.
Don’t hesitate to ask for explanations if medical terms or procedures are unclear. Understanding the treatment plan helps you feel more in control and better equipped to support your loved one.
Consider designating one family member as the main contact with the healthcare team. This can streamline information sharing and reduce stress. How can you organize your support system to keep everyone informed?

Credit: www.magonlinelibrary.com
Frequently Asked Questions
How Long Do Pneumonia Patients Stay On A Ventilator?
Pneumonia patients typically stay on a ventilator for 7 to 14 days. Duration depends on pneumonia severity and patient response. Some recover faster, while others need longer support for breathing. Doctors assess daily to decide ventilator removal safely.
What Factors Affect Ventilator Duration For Pneumonia?
Ventilator duration depends on pneumonia severity, age, overall health, and immune response. Complications like sepsis or lung damage can extend ventilator use. Early treatment and effective care reduce ventilation time and improve recovery chances.
Can Pneumonia Patients Recover Fully After Ventilator Use?
Yes, many pneumonia patients recover fully after ventilator support. Recovery depends on lung damage extent and timely treatment. Rehabilitation and follow-up care help restore lung function and overall health after ventilation.
When Is Ventilator Removal Safe For Pneumonia Patients?
Ventilator removal is safe once patients breathe independently without distress. Doctors evaluate oxygen levels, lung function, and strength before removal. Gradual weaning trials help ensure readiness for breathing without machine support.
Conclusion
Time on a ventilator for pneumonia varies by patient. Some recover quickly, while others need longer support. Doctors watch closely to decide when to remove the ventilator. Recovery depends on age, health, and pneumonia severity. Staying calm and following medical advice helps patients heal faster.
Understanding this process reduces fear and builds trust. Every case is different, so patience is key. Ventilator use aims to help breathing until lungs improve. This support can save lives and aid full recovery.